Causes and Risk Factors of Capgras Syndrome
The exact cause of Capgras syndrome is not fully understood, but several factors have been identified.
Neurological causes
Brain injuries, neurodegenerative diseases, or structural abnormalities can disrupt the neural pathways involved in facial recognition and emotional processing.
Psychiatric conditions
Capgras syndrome is commonly reported in individuals with schizophrenia or other psychotic disorders, where delusions and misinterpretations of reality are common.³
Cognitive and perceptual disruptions
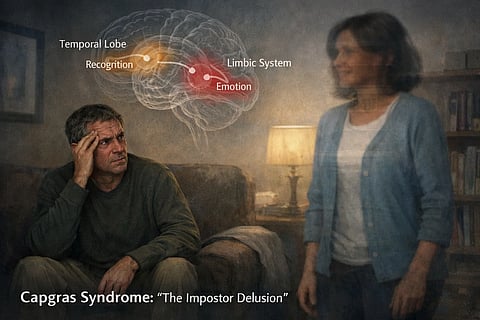
Research suggests the condition may result from impaired integration between:
When these systems fail to communicate properly, the brain may interpret familiar faces as unfamiliar, leading to the delusion.