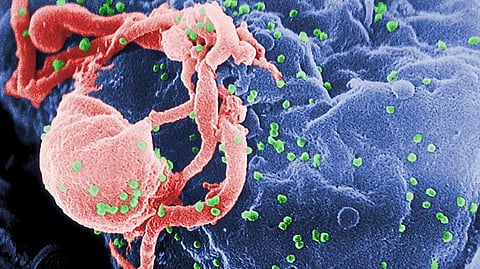
These children have a higher risk of poor health outcomes compared with those unexposed to HIV. Globally, studies have found that kids who have been exposed to HIV experience poorer growth and survival outcomes, however, little is known about this phenomenon.
The researchers also evaluated how the timing of maternal HIV infection and the type of antiretroviral therapy being provided during pregnancy might affect maternal inflammatory biomarkers. They found that the timing of when mothers became HIV infected and certain antiretroviral medications impacted several maternal inflammatory biomarkers.
The study, among the first to examine the impact of maternal inflammation and immune activation during pregnancy in people with HIV on their babies, analyzed data from 188 pregnant people with HIV from the Dynamic Cohort of the Surveillance Monitoring for ART Toxicities study conducted by the Pediatric HIV/AIDS Cohort Study (PHACS) network and 76 pregnant people without HIV from a cohort in New York. Of the pregnant people with HIV, 39 had acquired HIV perinatally, while 149 had acquired HIV later in life.